Waking up with a headache can interfere with concentration, energy, and daily routines. When this discomfort appears on most mornings and gradually eases as the day progresses, it may point to changes occurring during sleep rather than daytime activity. This pattern is often seen in people with sleep apnea, where breathing instability during sleep affects oxygen balance and may prompt patients to seek sleep apnea treatment in Clute, TX, after appropriate evaluation.
Headaches linked to sleep-related breathing disturbances are often overlooked because they do not always resemble migraines or sinus-related pain. Understanding how interrupted airflow affects the body overnight can help patients recognize when persistent morning symptoms may require further professional assessment.
Explanation of Sleep Apnea
Sleep apnea is a sleep-related breathing condition marked by repeated reductions or pauses in airflow during sleep. These interruptions can result from airway narrowing or inconsistent neurological control of breathing. The obstructive form is diagnosed most often. It develops when the muscles that support the throat relax excessively during sleep, limiting airflow. As oxygen levels decline, the body briefly arouses to restore breathing. These arousals are typically not remembered, yet their frequent repetition prevents normal progression through deeper stages of sleep.
Repeated disruption of airflow and oxygen regulation limits deep sleep stages that support neurological and cardiovascular recovery. Over time, this pattern may contribute to persistent daytime symptoms, including morning headaches.
How Sleep Apnea Causes Morning Headaches
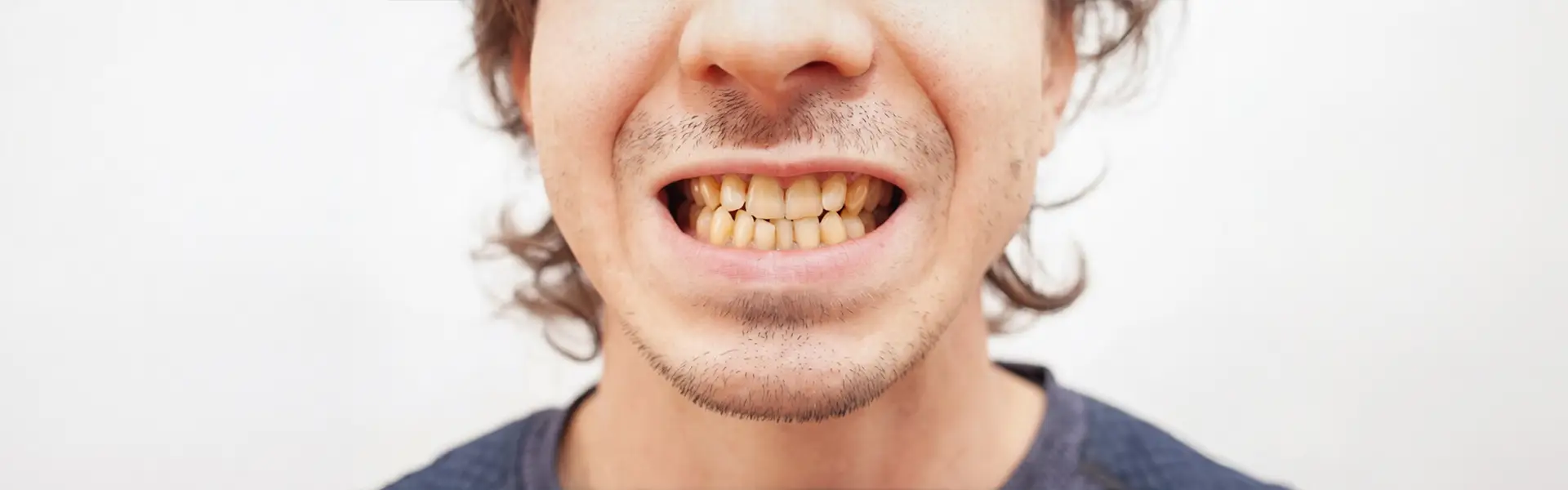
Headaches linked to sleep apnea often appear shortly after waking and gradually diminish within a few hours. Patients commonly describe the sensation as pressure-like rather than sharp or pulsating.
Reduced oxygen levels during sleep can influence cerebral blood flow, contributing to head discomfort in the morning. At the same time, interrupted breathing may allow carbon dioxide levels to rise, a physiological change associated with headache development. When sleep is repeatedly fragmented, normal pain-modulation pathways function less efficiently, which can increase sensitivity to head pain upon waking.
Jaw muscle tension and nighttime clenching frequently accompany airway instability. This added muscular strain may further contribute to discomfort involving the temples, jaw joints, or surrounding facial structures.
Other Signs Sleep Apnea May Be Affecting You
Morning headaches rarely exist on their own. Many adults with sleep apnea experience additional symptoms that develop gradually and may not initially seem connected.
Common findings include:
- Persistent or loud snoring
- Episodes of gasping or choking during sleep
- Dry mouth or throat irritation upon waking
- Ongoing daytime fatigue
- Reduced concentration or short-term memory changes
Oral findings may also be present. Tooth wear, jaw soreness, and signs of clenching can develop when airway instability increases muscle activity during sleep. During routine examinations, a dentist in Clute, TX, may identify these patterns and suggest further evaluation when they align with reported sleep-related concerns.
How Sleep Apnea Is Diagnosed
Assessment begins with a review of symptoms, sleep patterns, and overall health history. Clinicians evaluate factors such as snoring frequency, daytime alertness, and morning symptoms to determine whether diagnostic testing is appropriate.
Because breathing instability develops during sleep, objective testing is often necessary. Sleep studies monitor airflow, oxygen levels, heart rate, and sleep stages. Depending on individual circumstances, testing may be completed in a monitored sleep laboratory or through validated home-based studies.
When findings confirm a sleep-related breathing disorder, patients may be referred for sleep apnea treatment based on diagnostic results and overall health considerations. Management decisions rely on diagnostic findings and are coordinated with medical providers when appropriate.